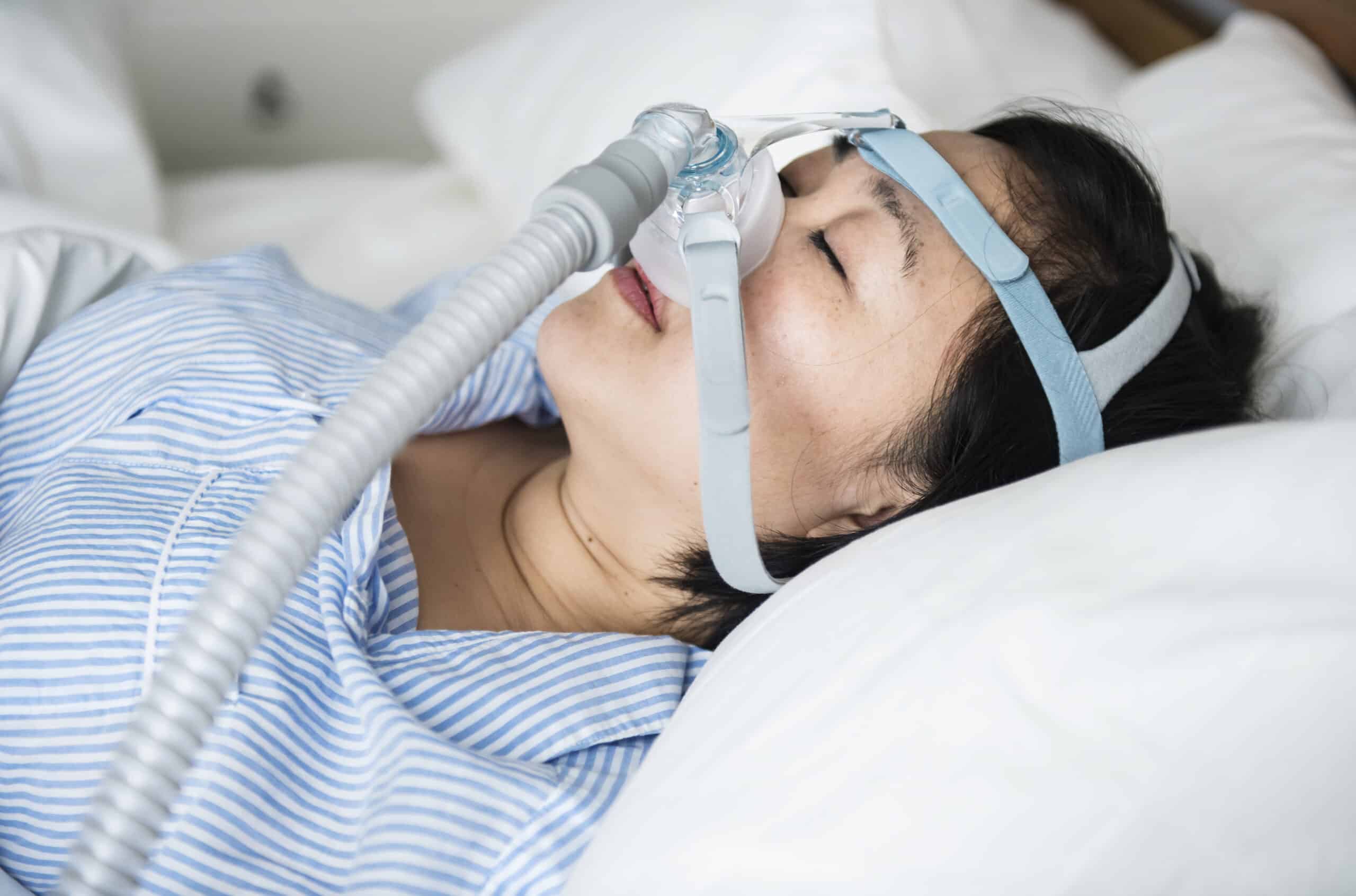
Sleep apnea is a serious sleep disorder in which breathing repeatedly stops during sleep, depriving the body of oxygen and disrupting sleep. For millions of patients in the United States, the question of whether sleep apnea can cause high blood pressure is a pressing health concern.
The answer, supported by extensive peer-reviewed research, is unequivocal: untreated sleep apnea is directly linked to elevated blood pressure, increased cardiovascular risk, and long-term damage to the cardiovascular system.
Table of Contents
How Sleep Apnea Affects the Cardiovascular System
There are different types of sleep apnea. Obstructive sleep apnea (OSA)—also referred to as obstructive sleep apnoea—is the most prevalent form, occurring when airway collapse blocks breathing during sleep. Central sleep apnea, a less common form of the condition, occurs when the brain fails to signal the respiratory muscles to breathe. In both cases, repeated episodes of breathing cessation lead to sustained drops in blood oxygen levels and trigger a cascade of physiological stress responses.
Each time you stop breathing during sleep, the body releases stress hormones that make the heart beat faster and tighten blood vessels. When this happens night after night, it leads to high blood pressure, weaker heart health, and a higher risk of heart problems like heart attacks and irregular heartbeats. This is why many people with sleep apnea also develop hard-to-treat high blood pressure, because the sleep problem continues every night.
Sleep apnea can harm your health in more ways than just high blood pressure. Untreated sleep apnea is linked to problems like the body not using insulin well, changes in how your body processes food, unhealthy blood vessels, too many harmful substances in the body, and extra body fluid. All these problems add up and make heart disease more likely in the long run.
What Peer-Reviewed Research Reveals About Hypertension and Obstructive Sleep Apnea
There is strong evidence linking obstructive sleep apnea and heart disease. A 2021 report from the American Heart Association showed OSA affects about 34% of middle-aged men and 17% of middle-aged women in the United States. In people who already have high blood pressure, heart failure, heart disease, irregular heartbeat, or stroke, OSA is even more common—between 40% and 80%. But it is still often not treated by heart doctors.
For patients with difficult-to-treat hypertension, the data are even more striking. Research in the Annals of the American Thoracic Society (2019) found OSA prevalence in cohorts with refractory hypertension ranges from 64% to 83%—confirming how frequently an untreated sleep disorder drives failed blood pressure control.
Recognizing the Signs of Sleep Apnea
Identifying sleep apnea symptoms early is the first step toward protecting sleep health and cardiovascular health.
Common symptoms include:
-
Loud snoring, often first noticed by a bed partner
-
Witnessed breathing stop during sleep
-
Excessive daytime sleepiness and daytime drowsiness
-
Morning headaches and dry mouth upon waking
-
Sleep deprivation and poor-quality, unrestful sleep
-
Difficulty concentrating and mood changes
Key risk factors include excess weight, family history of sleep disorders, and structural airway characteristics.
It is recommended that any individual presenting with these signs of sleep apnea alongside elevated blood pressure levels pursue formal evaluation. A sleep study or home sleep test—which measures the apnea-hypopnea index (AHI) to determine whether a patient has moderate or severe OSA—is the established diagnostic pathway.
Sleep Apnea Treatment Options and Blood Pressure Control
Treating sleep apnea produces measurable improvements in cardiovascular health and blood pressure control. Lifestyle changes are an important first-line approach: weight loss, sleeping on the side, avoiding alcohol before bed, and maintaining a consistent sleep schedule can all reduce OSA severity. Research in the journal Sleep (2011) found that structured exercise lowers the AHI by 5 to 8 breathing events per hour in patients with severe OSA by improving airway muscle tone and reducing inflammation.
CPAP therapy remains the gold standard for treating sleep apnea. Consistent CPAP machine use produces clinically significant reductions in blood pressure and long-term cardiovascular risk. For patients who cannot tolerate CPAP, oral appliances are a highly effective alternative. Custom mandibular advancement devices maintain an open airway, improve blood oxygen levels, and promote better sleep. Surgical procedures remain an option in selected cases where other treatments have not provided sufficient relief.
Why Choose Bloom Dental of Arlington
At Bloom Dental of Arlington, our team understands the critical relationship between sleep medicine and long-term heart health.
Our very own, Dr. Ashkan Yousefi is a Diplomate of the American Board of Dental Sleep Medicine and works closely with sleep specialists to deliver individualized treatment for sleep apnea. If you have sleep apnea symptoms alongside uncontrolled blood pressure levels, professional evaluation can make a meaningful difference. Our practice provides custom oral appliances designed for comfort and compliance.
To schedule a consultation, contact Bloom Dental of Arlington today.